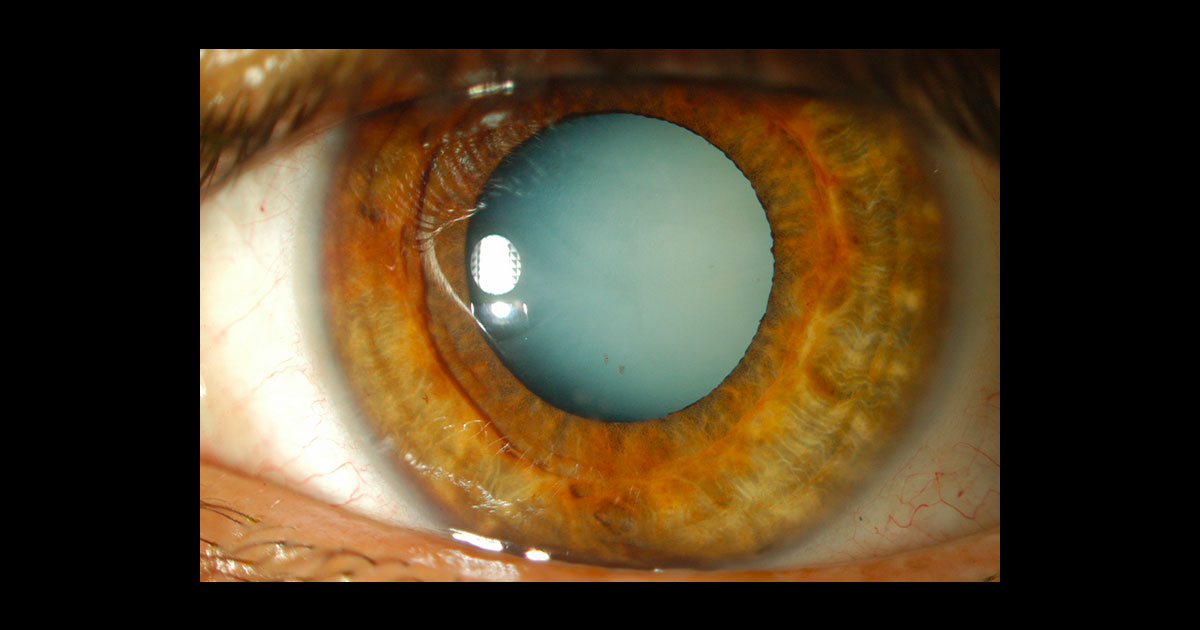
Figure 1: White cataract left eye
A 34 year male was referred with blurred vision in his left eye.
A 34 year old engineer was referred by his optometrist with blurred vision in the left eye which had been rapidly worsening over 4 months. His visual acuity was recorded at Right 6/5 and Left counting fingers. The examination demonstrated a white cataract in the left eye (Figure1). The right lens was clear.
What are the causes of unilateral cataract in a young adult?
- Traumatic
- Inflammatory
- Fuch's heterochromic iritis
- Chronic uveitis
- Retinal detachment
- Iatrogenic
- Idiopathic
Figure 2: B scan ultrasound was performed to exclude a retinal detachment
Close inspection revealed subtleiris heterochromia (Figure 3) and stellate keratic precipitates.
Figure 3: There is subtle left iris hypochromia
DIAGNOSIS
Fuch’s Heterochromic Cyclitis
After informed consent the patient underwent routine cataract surgery in the left eye. He had a monofocal lens implant with refractive target for distance.
Day 1 visual acuity of 6/7.5-. Postoperatively he used a standard regime of chloramphenicol, dexamethasone (Maxidex) and ketorolac (Acular) post operatively. At one month postoperatively acuity was 6/6+. Despite loss of accommodative function in the left eye he was still able to manage near tasks without glasses due to his right eye which still had good accommodative function.
Fuch’s heterochromic iridocyclitis (FHI) is an uncommon chronic unilateral uveitis. It is increasingly thought to be related to rubella infection. The hallmark signs are:
- Iris heterochromia and atrophy
- Keratic precipitates (usually stellate and pan corneal)
- Low-grade iridocyclitis
- Cataract in the absence of posterior synechiae
The inflammation in FHI is generally not responsive to corticosteroid eye drops. The main causes of vision loss in this condition are cataract, glaucoma and vitreous opacification. Caution is required during cataract surgery in FHI as there are often fragile iris vessels which cross the trabecular meshwork that are prone to rupturing during paracentesis of the globe. This can result in hyphaema. This is known as Amsler’s sign. Multifocal intraocular lenses are not recommended for these patients.
Tags: blurred vision, unilateral cataract, trauma, fuch's hereochromic iritis, retinal detachment